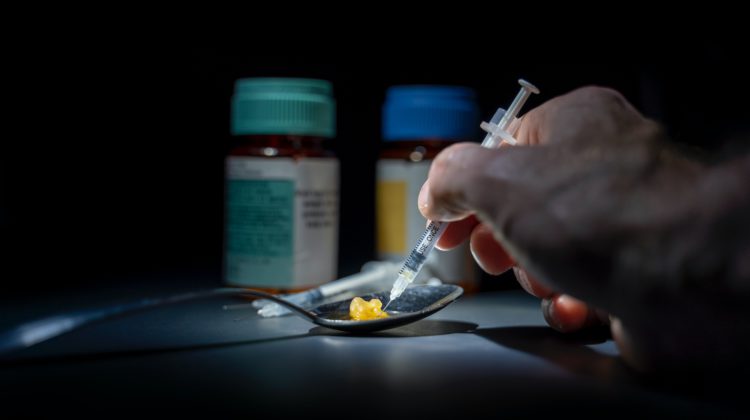
It’s been five years since British Columbia officially declared the overdose crisis a public health emergency.
Since 2016, 7,062 people have lost their lives to toxic drug supply.
Lisa Lapointe, B.C’s chief coroner, says in the following years, despite a number of actions taken at various levels of government, the province has continually set new records for illicit drug toxicity deaths.
A new record high was set last year with 1,724 lives lost, and in the first two months of 2021, another 329 people died because of illicit drugs.
The province says while virtually no area of B.C has been spared from the opioid crisis, First Nations communities have been particularly impacted.
The First Nations Health Authority (FNHA) reports between January and May 2020, 89 First Nations individuals died in B.C. due to illicit drug toxicity – a 93% increase compared to the same period in 2019.
During that period, 16 percent of all drug toxicity deaths in B.C. were Indigenous people, who account for just 3.3 percent of the province’s population.
“The opioid crisis continues to wreak havoc on Indigenous people five years after the B.C. government’s declaration of a public health emergency on opioid use is a clear indication that there is still much more to be done to resolve this tragic public health issue,” said Dr. Shannon McDonald, acting chief medical officer for the FNHA.
On the significant and somber anniversary, B.C says it is doing more to combat stigma and turn the tide on this crisis.
In a phone conference Wednesday morning, B.C’s Minister of Mental Health and Addictions Sheila Malcolmson said the province plans to officially request a federal exemption from Health Canada to decriminalize personal possession of drugs to remove the shame that often prevents people from reaching out for life-saving help.
“Stigma drives people to hide their drug use, avoid health care and use alone,” said Malcolmson.
“Through provincewide decriminalization, we can reduce the fear and shame that keep people silent about their drug use, and support people to reach out for help, life-saving supports and treatment.”
Some of the things the province plans to address in its work with the federal government will be defining simple possession, determining allowable drug amounts and ensuring the readiness of law enforcement, health and social services to support decriminalization.
During that conference, Malcomson was asked if the province plans to provide regulated drugs of choice for users at safe use sites instead of them getting it from the street.
She said “The framework around that is complex and detailed work. One that has to be done hand in hand with the medical community and always with patient safety at the forefront.”
“The health ministry is looking at securing a domestic supply of some drugs that haven’t been available before. So we have a lot of work ahead of us on that. WIthin our federal framework the work has to be led by the medical community and continuing to do the detailed and careful work to expand the number of substances available to subscribers,” she explained.
B.C is also boosting funds to help expand overdose prevention services coming in the form of $45-million dollars over the next three years.
The province says this investment will help regional overdose responses by expanding overdose prevention services like inhalation sites.
Last year, nearly 3,000 overdoses were survived at overdose prevention services, with zero deaths recorded.